Macrolides
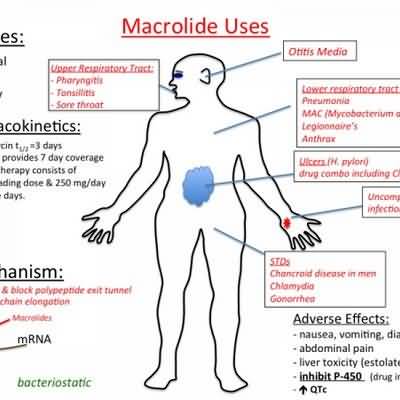
Macrolides
Macrolides are antibiotics. They are bacteriostatic or bactericidal in susceptible bacteria; they bind to cell membranes and cause changes in protein function, leading to bacterial cell death.
Indications
Treatment of acute infections caused by sensitive strains of Streptococcus pneumoniae, Mycoplasma pneumoniae, Listeria monocytogenes, Legionella pneumophila; URIs, lower respiratory tract infections, skin and soft-tissue infections caused by group A beta-hemolytic streptococci when oral treatment is preferred to injectable benzathine penicillin; PID caused by Neisseria gonorrhoeae in patients allergic to penicillin; intestinal amebiasis caused by Enta- moeba histolytica; infections in the newborn and in pregnancy that are caused by Chlamydia trachomatis and in adult chlamydial infections when tetracycline cannot be used; primary syphilis (Treponema pallidum) in penicillin-allergic patients; eliminating Bordetella pertussisorganisms from the nasopharynx of infected individuals and as prophylaxis in exposed and sus- ceptible individuals; superficial ocular infections caused by susceptible strains of microorganisms; prophylaxis of ophthalmia neonatorum caused by N. gonorrhoeaeor C. trachomatis In conjunction with sulfonamides to treat URIs caused by Haemophilus influenzae Adjunct to antitoxin in infections caused by Corynebacterium diphtheriaeand Coryne- bacterium minutissimum Prophylaxis against alpha-hemolytic streptococcal endocarditis before dental or other procedures in patients allergic to penicillin who have valvular heart disease and against infection in minor skin abrasions Adverse effects
in italics are most common; those in bold are life-threatening. U Do not crush. Unlabeled uses: Treatment of severe diarrhea associated with Campylobacter en- teritis or enterocolitis; treatment of genital, inguinal, or anorectal lymphogranuloma venereum infection; treatment of Haemophilus ducreyi (chancroid); treatment of acne vulgaris and skin infections caused by sensitive microorganisms Contraindications and cautions
Contraindicated with allergy to any macrolide antibiotic. Use cautiously with hepatic impairment or lactation (secreted and may be concentrated in breast milk; may modify bowel flora of breast-fed infant and interfere with fever workups). Adverse effects
CNS: Reversible hearing loss, confusion, uncontrollable emotions, abnormal think- ing, headache Dermatologic: Edema, urticaria, dermatitis, angioneurotic edema GI: Abdominal cramping, anorexia, diarrhea, vomiting, pseudomembranous coli- tis, hepatotoxicity Hypersensitivity: Allergic reactions ranging from rash to anaphylaxis Local: Irritation, burning, itchingat site of application Other: Superinfections Interactions
Drug-drug Increased serum levels of digoxin Increased effects of oral anticoagulants, theophyllines, carbamazepine Increased therapeutic and toxic effects of corticosteroids Increased levels of cyclosporine and risk of renal toxicity Increased irritant effects with peeling, desquamating, or abrasive agents used with dermatologic preparations Risk of prolonged QT interval if combined with other drugs that prolong QT interval Drug-lab test Interferes with fluorometric determination of urinary catecholamines Decreased urinary estriol levels caused by inhibition of hydrolysis of steroids in the gut Nursing considerations
Assessment
History: Allergy to macrolides, hepatic impairment, lactation, viral, fungal, mycobacterial infections of the eye Physical: Site of infection, skin color, lesions; orientation, affect, hearing tests; R, adventitious sounds; GI output, bowel sounds, liver evaluation; culture and sensitivity tests of infection, urinalysis, LFTs Interventions
Culture site of infection before therapy. Administer oral erythromycin base or stearate on an empty stomach, 1 hr before or 2�3 hr after meals, with a full glass of water (oral erythromycin estolate, ethylsuccinate, and certain enteric-coated tablets; see manufacturer�s instructions; may be given with- out regard to meals). Administer drug around the clock to maximize therapeutic effect; scheduling may have to be adjusted to minimize sleep disruption. Black box
warning Monitor liver function in patients on prolonged therapy; serious toxicity can occur. Institute hygiene measures and treatment if superinfections occur. If GI upset occurs with oral therapy, some preparations (see previous) may be given with meals, or it may be possible to substitute one of these preparations. Provide frequent small meals if GI problems occur. Establish safety measures (accompany patient, side rails) if CNS changes occur. Give patient support and encouragement to continue with therapy. Wash affected area, rinse well, and dry before topical application. Teaching points
Take oral drugs on an empty stomach, 1hr before or 2�3 hrs after meals, with a full glass of water, or, as appropriate, drug may be taken without regard to meals. These drugs should be taken around the clock; schedule to minimize sleep disruption. It is important that you finish the full courseof the drug therapy. Wash and rinse area and pat it dry before applying topical solutions; use fingertips or an applicator; wash hands thoroughly after application. You may experience these side effects: Stom- ach cramping, discomfort (taking the drug with meals, if appropriate, may alleviate this problem); uncontrollable emotions, crying, laughing, abnormal thinking (will end when the drug is stopped). Report severe or watery diarrhea, severe nau- sea or vomiting, dark urine, yellowing of the skin or eyes, loss of hearing, skin rash or itching. Representative drugs
azithromycin clarithromycin erythromycin fidaxomicin