UVEITIS
UVEITIS
ESSENTIALS OF DIAGNOSIS
General Considerations
Intraocular inflammation (uveitis) is classified as acute or chronic and as nongranulomatous or granulomatous, according to the clinical signs, and by its involvement of the anterior, intermediate, posterior, or all (panuveitis) segments of the eyeThe common types are acute nongranu- lomatous anterior, granulomatous anterior, and posterior
In most cases the pathogenesis of uveitis is primarily immunologic, but infection may be the cause, particularly in immunodeficiency states
The systemic disorders associated with acute nongranulomatous anterior uveitis are the HLA-B27-related conditions (ankylosing spondylitis, reactive arthritis, psoriasis, ulcerative colitis, and Crohn disease)
Chronic nongranulomatous anterior uveitis occurs in juvenile idiopathic arthritis
Behçet syndrome produces both anterior uveitis, with recurrent hypopyon but little discomfort, and posterior uveitis, characteristically with branch retinal vein occlusions
Both herpes simplex and herpes zoster infections may cause nongranulomatous anterior uveitis as well as retinitis (acute retinal necrosis)
Diseases producing granulomatous anterior uveitis also tend to be causes of posterior uveitis
These include sarcoidosis, toxoplasmosis, tuberculosis, syphilis, Vogt Koyanagi-Harada disease (bilateral uveitis associated with alopecia, poliosis [depigmented eyelashes, eyebrows, or hair], vitiligo, and hearing loss) , and sympathetic ophthalmia that occurs after penetrating ocular trauma
In toxoplasmosis, there may be evidence of previous episodes of retinochoroiditis
Syphilis characteristically produces a “salt and pepper” fundus but may present with a wide variety of clinical manifestations
The other principal pathogens responsible for ocular inflammation in HIV infection are cytomegalovirus (CMV), herpes simplex and herpes zoster viruses, mycobacteria, Cryptococcus, Toxoplasma, and Candida
Retinal vasculitis and intermediate uveitis predomi- nantly manifest as posterior uveitis with central or peripheral retinal abnormalities in retinal vasculitis and far peripheral retinal abnormalities (pars planitis) in intermediate uveitis
Retinal vasculitis can be caused by a wide variety of infectious agents and noninfectious systemic conditions but also may be idiopathic
Intermediate uveitis is often idiopathic but can be due to multiple sclerosis or sarcoidosis
Clinical Findings
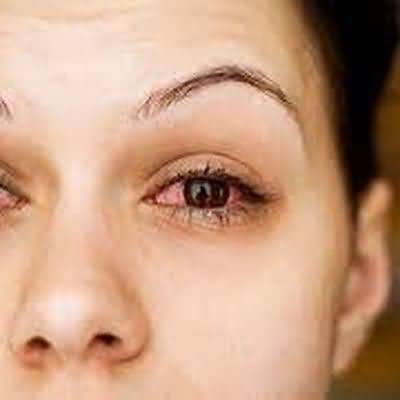
Anterior uveitis is characterized by inflammatory cells and flare within the aqueousIn severe cases, there may be hypopyon (layered collection of white cells) and fibrin within the anterior chamber
Cells may also be seen on the corneal endothelium as keratic precipitates (KPs)
In granulomatous uveitis, there are large “mutton-fat” KPs, and sometimes iris nodules
In nongranulomatous uveitis the KPs are smaller with no iris nodules
The pupil is usually small, and with the development of posterior synechiae (adhesions between the iris and anterior lens capsule) it also becomes irregular
Nongranulomatous anterior uveitis tends to present acutely with unilateral pain, redness, photophobia, and visual loss
However, in juvenile idiopathic arthritis there tends to be an indolent, often initially asymptomatic process with a high risk of sight-threatening complications
Granulomatous anterior uveitis is usually indolent, causing blurred vision in a mildly inflamed eye
In posterior uveitis, there are cells in the vitreous and there may be inflammatory retinal or choroidal lesions
Fresh retinal lesions are yellow with indistinct margins and there may be retinal hemorrhages, whereas older lesions have more definite margins and are commonly pigmented
Retinal vessel sheathing may occur adjacent to such lesions or more diffusely
In severe cases, vitreous opacity precludes visualization of retinal details
Posterior uveitis tends to present with gradual visual loss in a minimally inflamed eye
Bilateral involvement is common
Visual loss may be due to vitreous haze and opacities, inflammatory lesions involving the macula, macular edema, retinal vein occlusion, or rarely optic neuropathy
Differential Diagnosis
Retinal detachment, intraocular tumors, and central nervous system lymphoma may all masquerade as uveitisTreatment
Anterior uveitis usually responds to topical corticoste- roidsOccasionally periocular corticosteroid injections or even systemic corticosteroids are required
Dilation of the pupil is important to relieve discomfort and prevent permanent posterior synechiae
Posterior uveitis more com- monly requires systemic, periocular, or intravitreal corticosteroid therapy and occasionally systemic immunosuppression with agents such as azathioprine, cyclosporine, mycophenolate, methotrexate, tacrolimus, or sirolimus, of which some can be administered by intraocular injection
The use of biologic therapies is increasing
Pupillary dilation is not usually necessary
If an infectious cause is identified, specific antimicrobial therapy is often needed
In general, the prognosis for anterior uveitis, particularly the nongranulomatous type, is better than for posterior uveitis
When to Refer